Translational Pulmonary
& Immunology Research Center
& Immunology Research Center
Menu
TPIRC, Translational Pulmonary and Immunology Research Center, was established in 2015 by Dr. Inderpal Randhawa. Early in his career, Dr. Randhawa dedicated his career to challenging conventional approaches to treating life-threatening food allergies, and now multiple rare diseases. This challenge involved meticulously studying vast amounts of genetic and environmental data to develop personalized, data-driven treatment plans for each patient. This multi-system approach yielded an unprecedented success rate, allowing countless food-allergic individuals, particularly children and young adults, to safely enjoy foods that were once considered dangerous.
TPIRC’s success wasn’t limited to food allergies. Dr. Randhawa’s innovative model, built on precision medicine and data analysis, proved effective in tackling a wider range of complex and often rare diseases. This unique approach led TPIRC to become a safe and trustful clinic and research center for patients facing the challenges of rare and orphan diseases.

Our mission is two-fold: to advance treatment discovery at a pace that helps our patients today while building a scalable model of success to accelerate the rate of research discovery for all diseases.
To harness the power of big data to unravel the mysteries of rare diseases and deliver cures that restore hope and health to patients and families around the world.
Our pipeline echoes our mission and vision – to advance treatment discovery at a pace that helps our patients today while building a scalable model of success to accelerate the rate of research discovery for rare and orphan diseases.
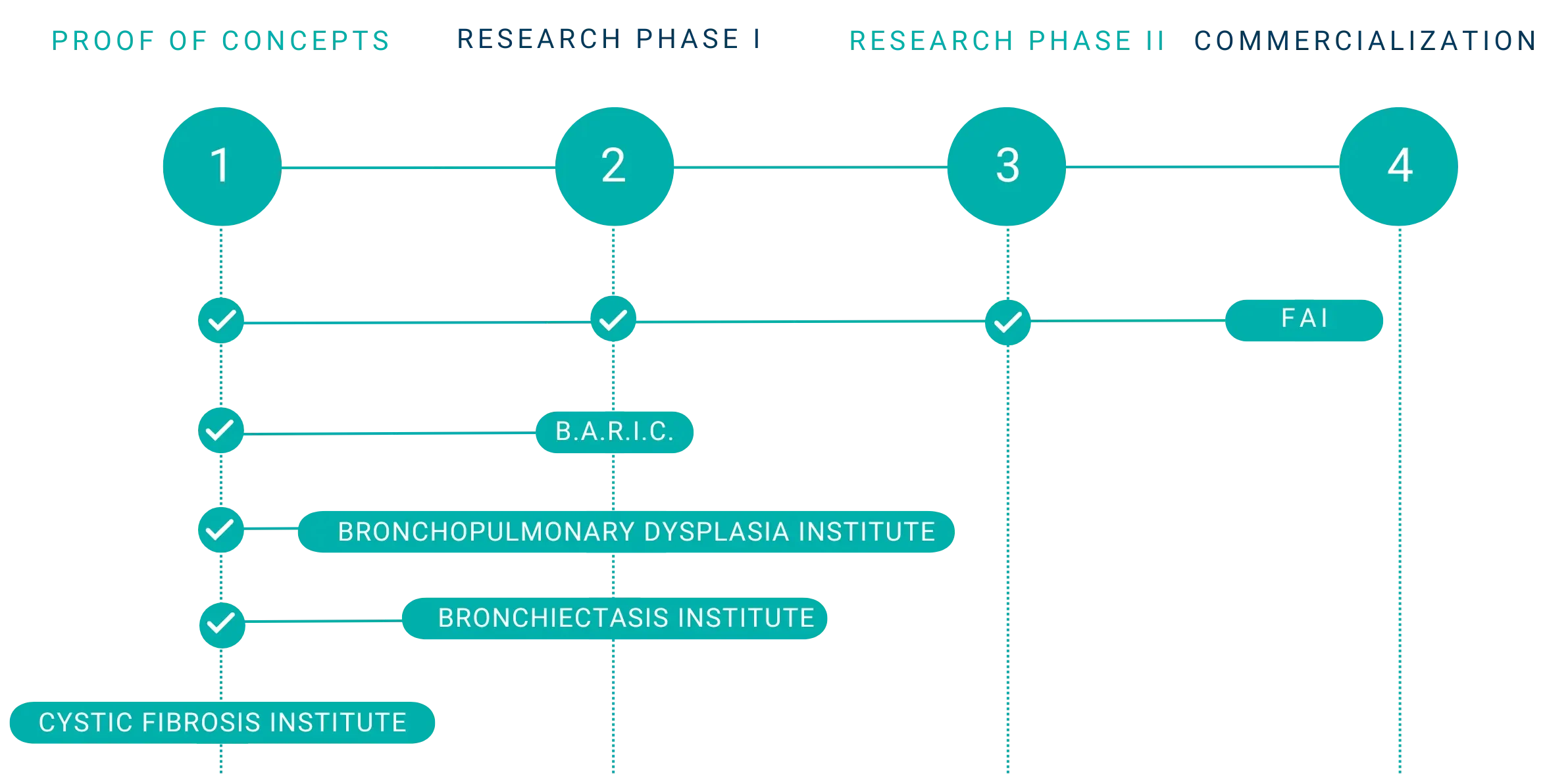
TPIRC is consistently developing advanced technology, proprietary artificial intelligence and machine learning algorithms, and efficient clinical environments to create significant impact in its 5 areas of focus.


Fueled by TPIRC’s groundbreaking research, the Tolerance Induction Program™ (TIP) at the Food Allergy Institute is revolutionizing food allergy treatment. With its high success rate and thousands achieving remission (meaning they can consume food without allergic reactions), this safe and innovative approach has transformed the lives of its patients. Following the principles of individualized treatment plans, AI-powered guidance, and clinical guidance, TIP is quickly revolutionizing how we approach healthcare. In the spirit of progression, we are:
The TIP Program has proved to be a beacon of hope for those seeking food freedom.

TPIRC is proud to be associated with Lung and Allergy Health Associates (LAHA) – a coordinated organization of physicians and healthcare groups focused on patient care and innovation.
TPIRC Diagnostics (formerly Foundation Labs) is the only allergy and pediatric pulmonary diagnostic lab in the nation. It is a blood draw center as well as a sample processing and lab testing center.
TPIRC researchers are developing tools to predict lung function decline and disease progression in Cystic Fibrosis (CF) patients. This is crucial because such a decline can lead to serious complications like lung transplants. Current methods for assessing CF severity are complex and don’t predict this decline. TPIRC’s study analyzes data from patients to identify factors linked to a significant drop in lung function. Based on analysis, we’ve developed a scoring system called the CF RD-Pro score, which considers factors like body mass index and Staphylococcus aureus infection, both potentially modifiable to slow down disease progression. Identifying high-risk patients using this score allows for earlier intervention and potentially better outcomes. The simplicity of the CF RD-Pro score also makes it practical for use in clinical settings.

Each year, thousands of premature babies face a lung condition called Bronchopulmonary Dysplasia (BPD) that makes breathing difficult. This is often due to a lack of a special substance called surfactant in their tiny air sacs. Currently, doctors use a machine with added surfactant to help these babies breathe, but long-term effects of this treatment are still being studied. Our research is looking for new ways to help by studying lung function in mice and exploring the genes involved in lung development. By understanding these areas, we hope to discover better and longer-lasting treatments for babies with BPD. We currently have 2 projects involving BPD. One measures lung function by comparing mice in an oxygen-rich environment with applied treatment to the non-manipulated control environment. The next creates a gene knockout model to understand alveoli secondary septa formation (invagination) event and the genes that control the process. We hope to impact the world of bronchopulmonary dysplasia by allowing the scientific community to:
Each patient receives a tailored treatment plan where they are prescribed personalized regimens based on their specific immune snapshot profile (e.g., three spoons of peanut butter weekly, etc.). We are using food science to create bars, bites, tarts, and gummies that contain major food allergens for easy and safe dosing. These bars impact those in the program and those in remission. This process includes scientific research to stabilize the proteins from allergens and ensure safe consumption. In turn, this creation will increase program retention, convenience, and compliance with treatment regimens.

At TPIRC, we believe that groundbreaking treatments shouldn’t be out of reach for anyone. That’s why we’re dedicated to ensuring equitable access to healthcare, regardless of financial limitations or geographical location. We’ve established three grant programs – the Military Grant, Diversity Grant, and Patient Care Fund – to bridge the gap and promote health equity.
Our commitment extends beyond financial barriers. We understand that rare diseases like those we focus on often receive little attention. That’s why we actively partner with our patients to champion their cause in legal, medical, and social arenas. We believe in empowering our patients and giving them a voice to advocate for themselves and others facing similar challenges.


The TPIRC butterfly logo represents the hope our institute offers to orphan diseases. Lifting this butterfly are wings representing lungs composed of many smaller circular segments. The lungs are the most critical organ to live. The lungs are composed of many vital connections to other areas of the body’s composition of health. Each circle exemplifies important disease areas that affect human health.
TPIRC is organized around a complete and comprehensive analysis of numerous data points studying many of these critical connections that yield health. TPIRC’s model of disease research, discovery, and therapy is not limited to any one disease. However, the butterfly’s wings are highlighted by five blue circles representing Dr. Randhawa’s sentinel interests: food anaphylaxis, bronchiectasis, cystic fibrosis, immune deficiency, and airway inflammatory disorders. TPIRC’s success in an array of diseases reflects its ultimate goal — to leave no disease behind.
